-
Statistical department’s site
Home page
Our publications
Chapter 9
Services for elderly dependent people (Note 1)
Future developments in the population mean Europe will have to face up to significant economic and social challenges. In particular demographic ageing will lead to an increase in public expenditure on pensions, social and health care, and other services needed to guarantee the elderly a good quality of life.
Life expectancy has increased and elderly people's health is generally good, and constantly improving. Preventative measures and health education mean that the elderly are aware of the importance of investing in their health and of following a healthy lifestyle to ward off the negative effects of old age. In Veneto, the elderly claim that they are very or quite satisfied with their health (68%) and the number of people who consider themselves to be in good health is greater than the number who state that they are in poor health, more than at a national level. A total of 42% of people aged 65-74 states that they are well or very well, while 16% state that they are in poor health. The remaining people claim to be neither well nor ill. As people grow older, from 75 years onwards, the percentage of people claiming to be in good health drops (22%), while most elderly people (52%) state that they are neither in good nor poor health. More frequently women have a more negative perception of their own health and the difference compared to men increases with age.
Even though being elderly, therefore, does not necessarily mean being ill or disabled, there is an association between old age and the onset of degenerative illnesses, reliance on care and disability, especially for the very elderly. For example, in Veneto, 68% of people aged 75 or over suffer from two or more chronic degenerative illnesses. They therefore see their quality of life worsening in terms of the reduction or loss of independence in everyday activities. A total of 46% of people aged 65-74 has multiple chronic degenerative illnesses.
Although life expectancy is, in fact, longer, it is also true that elderly people will become reliant on care in the latter part of their lives, and the period of time between losing autonomy and death is bound to become even longer over time.
This means that good health planning is concerned not only with increasing life expectancy, but also with ensuring good health in these extra years of life, so that the elderly can be active and independent. The financial effects are also positive. In fact according to an EU estimate (Note 2), in the optimistic hypothesis that life expectancy with good health conditions evolves in the same way as life expectancy, the foreseen increase in age-related healthcare expenditure would be almost halved. However, as in the future the over-80s will be the most rapidly growing age group, public expenditure for long-term assistance will rise considerably. It should also be noted that a considerable share of total healthcare expenditure during a person's life occurs towards the end of it.
When health conditions limit an elderly person's independence, currently it is usually the person's children who take care of him or her, which fills the gap in the State's welfare system. The Italian model of welfare has, in fact, always been based upon the availability of the family to provide emotional and concrete support to its most vulnerable members; in this way the family continues to act as a type of 'social shock absorber', protecting its members from situations of weakness and during critical stages in life. But if in the past the elderly could count on their numerous children and the non-working women in the house, many of the elderly people of tomorrow will be without an extended family network, in particular in the case of families that have broken up. It is undeniable, then, that the family will not always be able to meet the demands of caring for their elderly members, who will have to rely on outside care.
The future of health expenditure therefore not only depends on the ageing population, but also on the incidence of elderly people with disabilities and on an imbalance between formal and informal treatment, not to mention the type of services that the healthcare system intends to provide: residential care, semi-residential care, and home care, which may be provided as financial support or as services. Veneto's care network for elderly dependent people is the result of policies which, over the years, have led to a range of measures geared towards a complex social and healthcare situation. The increase in the quality and quantity of the services over the years has led to a rise in regional expenditure which is higher than the cost of living and than demographic trends. Population ageing is therefore drawing attention to the sustainability of policies for dependent people aged over-65.
Life expectancy has increased and elderly people's health is generally good, and constantly improving. Preventative measures and health education mean that the elderly are aware of the importance of investing in their health and of following a healthy lifestyle to ward off the negative effects of old age. In Veneto, the elderly claim that they are very or quite satisfied with their health (68%) and the number of people who consider themselves to be in good health is greater than the number who state that they are in poor health, more than at a national level. A total of 42% of people aged 65-74 states that they are well or very well, while 16% state that they are in poor health. The remaining people claim to be neither well nor ill. As people grow older, from 75 years onwards, the percentage of people claiming to be in good health drops (22%), while most elderly people (52%) state that they are neither in good nor poor health. More frequently women have a more negative perception of their own health and the difference compared to men increases with age.
Even though being elderly, therefore, does not necessarily mean being ill or disabled, there is an association between old age and the onset of degenerative illnesses, reliance on care and disability, especially for the very elderly. For example, in Veneto, 68% of people aged 75 or over suffer from two or more chronic degenerative illnesses. They therefore see their quality of life worsening in terms of the reduction or loss of independence in everyday activities. A total of 46% of people aged 65-74 has multiple chronic degenerative illnesses.
Although life expectancy is, in fact, longer, it is also true that elderly people will become reliant on care in the latter part of their lives, and the period of time between losing autonomy and death is bound to become even longer over time.
This means that good health planning is concerned not only with increasing life expectancy, but also with ensuring good health in these extra years of life, so that the elderly can be active and independent. The financial effects are also positive. In fact according to an EU estimate (Note 2), in the optimistic hypothesis that life expectancy with good health conditions evolves in the same way as life expectancy, the foreseen increase in age-related healthcare expenditure would be almost halved. However, as in the future the over-80s will be the most rapidly growing age group, public expenditure for long-term assistance will rise considerably. It should also be noted that a considerable share of total healthcare expenditure during a person's life occurs towards the end of it.
When health conditions limit an elderly person's independence, currently it is usually the person's children who take care of him or her, which fills the gap in the State's welfare system. The Italian model of welfare has, in fact, always been based upon the availability of the family to provide emotional and concrete support to its most vulnerable members; in this way the family continues to act as a type of 'social shock absorber', protecting its members from situations of weakness and during critical stages in life. But if in the past the elderly could count on their numerous children and the non-working women in the house, many of the elderly people of tomorrow will be without an extended family network, in particular in the case of families that have broken up. It is undeniable, then, that the family will not always be able to meet the demands of caring for their elderly members, who will have to rely on outside care.
The future of health expenditure therefore not only depends on the ageing population, but also on the incidence of elderly people with disabilities and on an imbalance between formal and informal treatment, not to mention the type of services that the healthcare system intends to provide: residential care, semi-residential care, and home care, which may be provided as financial support or as services. Veneto's care network for elderly dependent people is the result of policies which, over the years, have led to a range of measures geared towards a complex social and healthcare situation. The increase in the quality and quantity of the services over the years has led to a rise in regional expenditure which is higher than the cost of living and than demographic trends. Population ageing is therefore drawing attention to the sustainability of policies for dependent people aged over-65.
In just eight years, from 2001 to 2009, the population in Veneto rose by more than 382,000 inhabitants. Of these, 38.7% were aged over 65 and were therefore classified as "elderly". 24% were aged 75 and over. These are sigificant figures as in Veneto the over-65s make up almost 20% of the population, with 9.6% aged 75 or over.
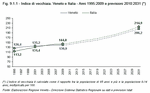
A further indicator tells us how much the population is ageing. The ageing index is measured in percent by dividing the number of inhabitants aged over 65 by the number of members of the population aged 0 to 14 years. In Veneto this index was 126.4% in 1995 and 135.2% in 2001. In 2009 it was 139.9%, while the figure for Italy was 144%. (Figure 9.1.1)
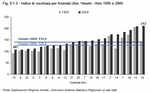
In the regions covered by the various Local Health Authorities (ULSS) in Veneto, the ageing index varies significantly. In 2009 Local Health Authority of Alta Padovana (ULSS 15) was the youngest area with an ageing index of 107%, followed by Asolo (ULSS 8) at 107.5%, while the oldest area is Adria (ULSS 19), with an index of 212%, slightly higher than that of Veneziana (ULSS 12) at 208.7%. (Figure 9.1.2)
Demographic estimates provided by Italy's National Institute of Statistics (ISTAT) indicate that in 2021 and 2031 the number of elderly people in Veneto will be 22.5% and 26.5% respectively. The share of elderly people will therefore continue to rise because of longer life expectancy. Moreover, the share of young people is expected to decrease. Therefore there will be a population imbalance leading to increasingly complex challenges for the region's Healthcare System. (For a more in-depth discussion of population ageing see Chapter 7).
A further indicator tells us how much the population is ageing. The ageing index is measured in percent by dividing the number of inhabitants aged over 65 by the number of members of the population aged 0 to 14 years. In Veneto this index was 126.4% in 1995 and 135.2% in 2001. In 2009 it was 139.9%, while the figure for Italy was 144%. (Figure 9.1.1)
In the regions covered by the various Local Health Authorities (ULSS) in Veneto, the ageing index varies significantly. In 2009 Local Health Authority of Alta Padovana (ULSS 15) was the youngest area with an ageing index of 107%, followed by Asolo (ULSS 8) at 107.5%, while the oldest area is Adria (ULSS 19), with an index of 212%, slightly higher than that of Veneziana (ULSS 12) at 208.7%. (Figure 9.1.2)
Demographic estimates provided by Italy's National Institute of Statistics (ISTAT) indicate that in 2021 and 2031 the number of elderly people in Veneto will be 22.5% and 26.5% respectively. The share of elderly people will therefore continue to rise because of longer life expectancy. Moreover, the share of young people is expected to decrease. Therefore there will be a population imbalance leading to increasingly complex challenges for the region's Healthcare System. (For a more in-depth discussion of population ageing see Chapter 7).
The region's administrational and legislative policies have always taken into account the increased demand for services for those reliant on care. Not only has there been an increase in the allocation of the regional budget, however, the organisation of the system has been reworked as well. In fact regional planning has confirmed that the integration of social and health care is an objective, along with the carrying out of its Local Area Plans. The best definition of regulations can be found in Article 124 of Regional Law LR 11/2001 which in defining its social services states: "Regione Veneto aims to integrate social services with health services in order to improve quality of life and the effectiveness of measures in order to maintain a state of wellbeing and prevent and remove causes of harm, disadvantage and illness. Regione Veneto protects health, in the widest meaning of the term, as a fundamental individual right which is in the interests of the community."
More recently, with the adoption of Regional Law LR 30/2009, the Regional fund for the non self-sufficient was introduced. This fund aims to guarantee a regional system of social and healthcare to those who are reliant on care, as well as to support care work by families.
The fund pools the resources of a previous fund that had been set up according to Article 3 of the 2008 Regional Financial Law, those allocated to a homecare fund by Article 26 of Regional Law LR 9/2005, those for alarm-call systems and remote surveillance, and the resources to finance day-centres for people with disabilities.
Contributions to the fund also come from the State or other public authorities from funding allocated to those reliant on care. To increase the sustainability of the services, Article 7 of Regional Law LR 30/2009 envisages other forms of revenue, including the introduction of a share of revenue from income tax. This has not yet been brought into effect.
The fund pools the resources of a previous fund that had been set up according to Article 3 of the 2008 Regional Financial Law, those allocated to a homecare fund by Article 26 of Regional Law LR 9/2005, those for alarm-call systems and remote surveillance, and the resources to finance day-centres for people with disabilities.
Contributions to the fund also come from the State or other public authorities from funding allocated to those reliant on care. To increase the sustainability of the services, Article 7 of Regional Law LR 30/2009 envisages other forms of revenue, including the introduction of a share of revenue from income tax. This has not yet been brought into effect.
This analysis focuses on policies for elderly dependent people. The assistance system provides both residential and home care.
The evolution of health policies means that admittance to hospital is only for critical phases of illnesses and follow-up treatment. The regional network of residential services deals with long-term treatment and lengthy rehabilitation. Health assistance that takes less than three hours is defined as "extensive". This is the kind of assistance that the structures in Veneto's non-hospital network deal with, outlined by Regional Government Decree DGR 51/2000 in three types of services characterised by medium levels of health assistance, known today as second-level care, and reduced and minimal care, today known as first-level care. There is one second-level place to every three first-level places.
This service was confirmed by Regional Government Decree DGR 464/2006, which updated regional planning of residential care. This also defined criteria for calculating the demand for care, a theoretical parameter which should be updated annually. It calculates the number of authorisations that can be assigned, as well as the number of bed places that can be authorised for each Local Health Authority. This number shows the relation between age groups and the care that can be provided in the area. In fact it is calculated by multiplying the age groups of inhabitants within each ULSS by the following coefficients:
Another new feature is the introduction of an authorisation for residential care (Note 4), which the user is given to access residential and semi-residential care. This guarantees the users and their families more freedom of choice. The new plan also considers care in the Alzheimer's High Protection Section (SAPA), in services for users in a Persistent Vegetative State (PVS) and temporary respite care in residential homes.
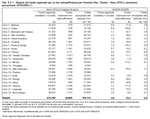
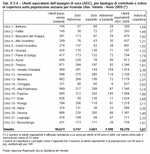
The assignment of authorisations for residential care also depends on the availability of regional budget in relation to demand, calculated as seen above. The alignment of this parameter is gradual, as in the past the assignment of authorisations to the Local Health Authorities also took into account the number of bed places in each area. Therefore, for some ULSS the number of authorisations is higher than the average regional parameter, and in others is lower. New authorisations may be allocated to the Local Health Authorities with a lower than average number to bridge the gap with the regional average. This change can be seen in the following table, which does not show the transfer of authorisations from ULSS 14 to ULSS 16 following the implementation of Regional Law LR 22/2008 on 1 January 2010. This shifted nine municipalities in the Saccisica area from ULSS 14 to ULSS 16. (Table 9.3.1)
For elderly dependent people in Veneto today there are 19,859 first-level care authorisations and 3,966 second-level care authorisations. Moreover there are 795 first-level places and 24 second-level places assigned to people of the Church who are not provided for by the residential care system and therefore not accounted for when calculating demand. There are 1,211 places in day-centres for the elderly, 150 for patients in the Alzheimer's High Protection Sections and 165 for those in a Persistent Vegetative State. (Table 9.3.2)
The relation between the number of authorisations and demand is on average 87 authorisations per 100 units of demand. Thirteen Local Health Authorities have more places and eight have fewer. (Figure 9.3.2)
Finally it is also important to consider the value of each authorisation for residential care, which together are defined as "healthcare shares". These are part of the value of the fee paid to the Local Health Authority for care in authorised residential homes, in relation to the type of service and the user's needs. They mainly cover expenses for care workers, nurses and social activities. The other part of the fee is the so-called "hotel share", which is paid directly by the user or by the municipality in some cases.
Authorisations for first- and second-level residential care account for most non-hospital residential care expenditure. From 2001 to 2010 their value rose respectively by 46%, from 33.57 euro to 49 euro, and by 54.9%, from 36.15 euro to 56 euro.
Multiplied by 365 days, the value per capita of a place in residential care in 2010 was 17,885 euro for first-level care and 20,440 euro for second-level care. (Figure 9.3.3)
Policies supporting home care are divided into three areas, as outlined in Regional Government Decree DGR 39/2006, which defines the "Local Plan for Home Care". These are:
As concerns services offered in the users' homes, Regional Government Decree DGR 39/2006 makes exclusive reference to social care services, which are provided by local authorities, and may be delegated to the ULSS as foreseen by the Local Area Plan. These services aim at prevention, maintainance and rehabilitation which will allow elderly dependent people to stay in their own home. They also offer support to their caregivers. The services are provided directly by the municipality, unless otherwise delegated by the Local Health Authority, and usually include the supply of meals, home help, transport, psychological and social support.
Home care services that offer assistance directly to the elderly person with home visits and nursing staff are part of the basic levels of regional assistance (Note 5). The objectives of these services depend both on the users and the human resources (Note 6). As concerns the users, the aim is to offer care to at least 2% of over-65s. In 2009 the figure for Veneto was 1.62%. (Figure 9.3.4)
As concerns the ratio between staff and users, the aim is to provide one worker (Note 7) working full-time for 6 to 14 users. The regional average in 2009 was 9.8 users per worker, with a low of 2.3 users for ULSS 12 and a high of 57.9 for ULSS 7. (Figure 9.3.5)
In 2009, 23,431 people were awarded a care allowance, also for a period of less than 12 months. There was the equivalent of 18,270 users, calculated as if all users had been awarded the allowance for exactly 12 months. Of these, 3,747 were awarded the highest allowance because they suffered from Alzheimer's or other forms of dementia leading to behavioural problems, 2,661 because they had a live-in carer, and 1,190 because they had both Alzheimer's and a live-in carer.
The average annual care allowance awarded was 2,822.41 euro; 4,527.44 euro for people with Alzheimer's; 3,257.27 euro for those with a live-in carer; 4,767.38 euro for those with Alzheimer's and a live-in carer; and an average of 1,898.50 euro for the remaining users.
There is also a coverage index for care allowance, which in any case is not an objective, as it does not require particular organisational resources. In 2009 there was an average of 1.87 equivalent users per 100 inhabitants aged 65 and over. (Table 9.3.4)
Respite care was set up in experimental form by Regional Government Decree DGR 3960/2001, with the aim of introducing forms of support for members of the family providing care. These services, known as "good service" and "good respite" allow the families to put their loved ones in temporary care or to make use of extra services other than those provided by the home care service.
This form of support stems from the need to respond rapidly to urgent requirements and is currently organised in different ways from one Local Health Authority to another, also depending on different regulations in Local Area Plans. It is therefore difficult to give an accurate analysis of its use.
Residential care
The most recent model for assistance to dependent persons who cannot be cared for at home is covered by Regional Government Decree DGR 751/2000. Following the reform of Italy's national health service, this completed the regional planning of residential homes offering health, medical, nursing and rehabilitation assistance. The evolution of health policies means that admittance to hospital is only for critical phases of illnesses and follow-up treatment. The regional network of residential services deals with long-term treatment and lengthy rehabilitation. Health assistance that takes less than three hours is defined as "extensive". This is the kind of assistance that the structures in Veneto's non-hospital network deal with, outlined by Regional Government Decree DGR 51/2000 in three types of services characterised by medium levels of health assistance, known today as second-level care, and reduced and minimal care, today known as first-level care. There is one second-level place to every three first-level places.
This service was confirmed by Regional Government Decree DGR 464/2006, which updated regional planning of residential care. This also defined criteria for calculating the demand for care, a theoretical parameter which should be updated annually. It calculates the number of authorisations that can be assigned, as well as the number of bed places that can be authorised for each Local Health Authority. This number shows the relation between age groups and the care that can be provided in the area. In fact it is calculated by multiplying the age groups of inhabitants within each ULSS by the following coefficients:
- 0.06% for the population in the 0-64 age group;
- 0.65% (+0.5% for mountain areas (Note 3) and the Venetian islands) for the population in the 65-74 age group;
- 4.40% (+1% for mountain areas and the Venetian islands) for population in the 75 and over age group.
Another new feature is the introduction of an authorisation for residential care (Note 4), which the user is given to access residential and semi-residential care. This guarantees the users and their families more freedom of choice. The new plan also considers care in the Alzheimer's High Protection Section (SAPA), in services for users in a Persistent Vegetative State (PVS) and temporary respite care in residential homes.
The assignment of authorisations for residential care also depends on the availability of regional budget in relation to demand, calculated as seen above. The alignment of this parameter is gradual, as in the past the assignment of authorisations to the Local Health Authorities also took into account the number of bed places in each area. Therefore, for some ULSS the number of authorisations is higher than the average regional parameter, and in others is lower. New authorisations may be allocated to the Local Health Authorities with a lower than average number to bridge the gap with the regional average. This change can be seen in the following table, which does not show the transfer of authorisations from ULSS 14 to ULSS 16 following the implementation of Regional Law LR 22/2008 on 1 January 2010. This shifted nine municipalities in the Saccisica area from ULSS 14 to ULSS 16. (Table 9.3.1)
For elderly dependent people in Veneto today there are 19,859 first-level care authorisations and 3,966 second-level care authorisations. Moreover there are 795 first-level places and 24 second-level places assigned to people of the Church who are not provided for by the residential care system and therefore not accounted for when calculating demand. There are 1,211 places in day-centres for the elderly, 150 for patients in the Alzheimer's High Protection Sections and 165 for those in a Persistent Vegetative State. (Table 9.3.2)
The relation between the number of authorisations and demand is on average 87 authorisations per 100 units of demand. Thirteen Local Health Authorities have more places and eight have fewer. (Figure 9.3.2)
Finally it is also important to consider the value of each authorisation for residential care, which together are defined as "healthcare shares". These are part of the value of the fee paid to the Local Health Authority for care in authorised residential homes, in relation to the type of service and the user's needs. They mainly cover expenses for care workers, nurses and social activities. The other part of the fee is the so-called "hotel share", which is paid directly by the user or by the municipality in some cases.
Authorisations for first- and second-level residential care account for most non-hospital residential care expenditure. From 2001 to 2010 their value rose respectively by 46%, from 33.57 euro to 49 euro, and by 54.9%, from 36.15 euro to 56 euro.
Multiplied by 365 days, the value per capita of a place in residential care in 2010 was 17,885 euro for first-level care and 20,440 euro for second-level care. (Figure 9.3.3)
Home care
The importance of keeping elderly dependent people in their own home environment is receiving increasing recognition. Therefore for some years, regional policies have aimed to enable people to stay at home, while residential care is only used for people who have no other option. Even within the home environment it is necessary to guarantee the quality and appropriateness of services, as well as their accessibility and sustainability.Policies supporting home care are divided into three areas, as outlined in Regional Government Decree DGR 39/2006, which defines the "Local Plan for Home Care". These are:
- services provided in the home to support the family, which must account for at least 20% of home care resources, i.e. social home care, health home care, including the supply of prostheses and aids, and integrated social and health care (SAD/ADI), alarm call systems and remote surveillance, services provided by the local community.
- financial support (at least 45% of the resources): care allowances (ADC) for the users and their families, which vary according to the type of care and the types of assistance provided ("basic" users, users with Alzheimer's, users with a live-in carer, and users with Alzheimer's and a live-in carer). Variations also depend on the user's equivalent financial situation indicator (ISEE), which must be lower than around 15,000 euro to be able to benefit.
- respite services for the family (at least 7% of the resources): temporary stays in residential care, holidays, etc. for dependent people.
As concerns services offered in the users' homes, Regional Government Decree DGR 39/2006 makes exclusive reference to social care services, which are provided by local authorities, and may be delegated to the ULSS as foreseen by the Local Area Plan. These services aim at prevention, maintainance and rehabilitation which will allow elderly dependent people to stay in their own home. They also offer support to their caregivers. The services are provided directly by the municipality, unless otherwise delegated by the Local Health Authority, and usually include the supply of meals, home help, transport, psychological and social support.
Home care services that offer assistance directly to the elderly person with home visits and nursing staff are part of the basic levels of regional assistance (Note 5). The objectives of these services depend both on the users and the human resources (Note 6). As concerns the users, the aim is to offer care to at least 2% of over-65s. In 2009 the figure for Veneto was 1.62%. (Figure 9.3.4)
As concerns the ratio between staff and users, the aim is to provide one worker (Note 7) working full-time for 6 to 14 users. The regional average in 2009 was 9.8 users per worker, with a low of 2.3 users for ULSS 12 and a high of 57.9 for ULSS 7. (Figure 9.3.5)
In 2009, 23,431 people were awarded a care allowance, also for a period of less than 12 months. There was the equivalent of 18,270 users, calculated as if all users had been awarded the allowance for exactly 12 months. Of these, 3,747 were awarded the highest allowance because they suffered from Alzheimer's or other forms of dementia leading to behavioural problems, 2,661 because they had a live-in carer, and 1,190 because they had both Alzheimer's and a live-in carer.
The average annual care allowance awarded was 2,822.41 euro; 4,527.44 euro for people with Alzheimer's; 3,257.27 euro for those with a live-in carer; 4,767.38 euro for those with Alzheimer's and a live-in carer; and an average of 1,898.50 euro for the remaining users.
There is also a coverage index for care allowance, which in any case is not an objective, as it does not require particular organisational resources. In 2009 there was an average of 1.87 equivalent users per 100 inhabitants aged 65 and over. (Table 9.3.4)
Respite care was set up in experimental form by Regional Government Decree DGR 3960/2001, with the aim of introducing forms of support for members of the family providing care. These services, known as "good service" and "good respite" allow the families to put their loved ones in temporary care or to make use of extra services other than those provided by the home care service.
This form of support stems from the need to respond rapidly to urgent requirements and is currently organised in different ways from one Local Health Authority to another, also depending on different regulations in Local Area Plans. It is therefore difficult to give an accurate analysis of its use.
Figure 9.3.1
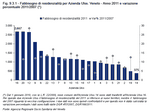
Table 9.3.1
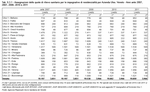
Table 9.3.2
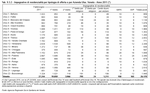
Figure 9.3.2
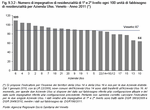
Figure 9.3.3
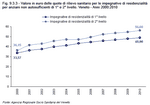
Table 9.3.3
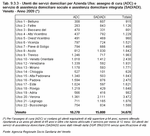
Figure 9.3.4
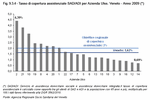
Figure 9.3.5
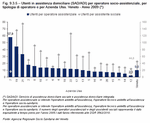
Table 9.3.4
How much do dependent people cost in Veneto? To answer this question the Regional Health Authority is carrying out a comparative study focusing on demand, regional funding and the costs of the services as revealed by the Local Health Authority accounts. These costs exceed the money available in the Non self-sufficiency fund and come out of healthcare expenditure. The results of this study will be published by 2011.
The data for regional funding are presented here, highlighting some trends with a focus on the most recent years. Regional Law LR 30/2009, mentioned earlier, set up the Regional non self-sufficiency fund by pooling a series of funds, starting with the one set up by Article 3 of Regional Law LR 1/2008 (Regional Finance Law). This fund is distributed annually, according to decisions made by the Board for the Regional Council, on the basis of criteria and indicators that are outlined by Regione Veneto.
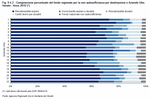
In 2009 and 2010, the first two financial years for the fund in conformity with Article 3 of Regional Law LR 1/2008, 680 million euro and 704 million euro respectively were allocated. Of these amounts, in both years 668,450 million euro came from the Regional Health Fund (FSR) and the remainder was mainly from State funding for non self-sufficiency. The way the fund was shared out was mostly similar in both years. In 2010 65% was allocated to residential care for the elderly; 13% to home care for the elderly and people with disabilities; 11% to day centres for people with disabilities; and 7% to residential care for people with disabilities. Finally 4% came from the national non self-sufficiency fund (Figure 9.4.1), (Figure 9.4.2) and (Table 9.4.1)
Between 2001 and 2008 about 6.4% of the FSR was allocated to non self-sufficiency. This increased significantly in 2009, rising to 8.7% from 481 million euro to 668 million euro. This was due to Article 3 of Regional Law LR 1/2008, which transferred resources allocated to day-centres for people with disabilities to the non self-sufficiency fund. Previously these had come from other health funds and those allocated to home care, which was part of the regional social fund. (Table 9.4.2)
Funding for residential services for elderly dependent people rose by 62% between 2001 and 2010, while the population aged 65 or over increased by 18% in the same period.
This figure should be considered along with the increase in the cost of living, as well as the quantitative increase in investment in residential services over the last decade. The upward trend has slowed done over the last two years to 2.4%. The reason for this is that in recent years regional policy has aimed to increase funding for home care, using all of the national non self-sufficiency fund to achieve this. Both services and financial support through the care allowance for families have increased. This has brought together financial contributions for those who take care of elderly dependent people at home, in particular those affected by behavioural problems. (Table 9.4.3)
The future holds a multifaceted challenge in store, caused both by the ageing population and the sustainability of the system. On the one hand it will be opportune, as well as fair, to reduce the differences in the services offered by the various Local Health Authorities, particularly as far as residential care is concerned. This could be brought about by compensating areas with fewer places in residential care with an increase in services for home care and direct financial contributions. On the other hand, it will lead to a new relationship between the funding of residential care and home care services. This calculation will perhaps be possible after having determined the entity of the resources in the healthcare fund, which today form part of the expenditure for non self-sufficiency. This is especially the case as far as both residential and home care of a nursing, rehabilitational and medical nature are concerned.
The data for regional funding are presented here, highlighting some trends with a focus on the most recent years. Regional Law LR 30/2009, mentioned earlier, set up the Regional non self-sufficiency fund by pooling a series of funds, starting with the one set up by Article 3 of Regional Law LR 1/2008 (Regional Finance Law). This fund is distributed annually, according to decisions made by the Board for the Regional Council, on the basis of criteria and indicators that are outlined by Regione Veneto.
In 2009 and 2010, the first two financial years for the fund in conformity with Article 3 of Regional Law LR 1/2008, 680 million euro and 704 million euro respectively were allocated. Of these amounts, in both years 668,450 million euro came from the Regional Health Fund (FSR) and the remainder was mainly from State funding for non self-sufficiency. The way the fund was shared out was mostly similar in both years. In 2010 65% was allocated to residential care for the elderly; 13% to home care for the elderly and people with disabilities; 11% to day centres for people with disabilities; and 7% to residential care for people with disabilities. Finally 4% came from the national non self-sufficiency fund (Figure 9.4.1), (Figure 9.4.2) and (Table 9.4.1)
Between 2001 and 2008 about 6.4% of the FSR was allocated to non self-sufficiency. This increased significantly in 2009, rising to 8.7% from 481 million euro to 668 million euro. This was due to Article 3 of Regional Law LR 1/2008, which transferred resources allocated to day-centres for people with disabilities to the non self-sufficiency fund. Previously these had come from other health funds and those allocated to home care, which was part of the regional social fund. (Table 9.4.2)
Funding for residential services for elderly dependent people rose by 62% between 2001 and 2010, while the population aged 65 or over increased by 18% in the same period.
This figure should be considered along with the increase in the cost of living, as well as the quantitative increase in investment in residential services over the last decade. The upward trend has slowed done over the last two years to 2.4%. The reason for this is that in recent years regional policy has aimed to increase funding for home care, using all of the national non self-sufficiency fund to achieve this. Both services and financial support through the care allowance for families have increased. This has brought together financial contributions for those who take care of elderly dependent people at home, in particular those affected by behavioural problems. (Table 9.4.3)
The future holds a multifaceted challenge in store, caused both by the ageing population and the sustainability of the system. On the one hand it will be opportune, as well as fair, to reduce the differences in the services offered by the various Local Health Authorities, particularly as far as residential care is concerned. This could be brought about by compensating areas with fewer places in residential care with an increase in services for home care and direct financial contributions. On the other hand, it will lead to a new relationship between the funding of residential care and home care services. This calculation will perhaps be possible after having determined the entity of the resources in the healthcare fund, which today form part of the expenditure for non self-sufficiency. This is especially the case as far as both residential and home care of a nursing, rehabilitational and medical nature are concerned.